From Small Habits to Meaningful Change: What 8 Weeks to 6 Months of Holly Health Can Do for Users with Anxiety and Depression
Anxiety and depression are among the most common long-term health challenges across the UK, affecting millions of individuals across all age groups (NHS, 2024; Mind,2023). Unlike many physical conditions, their impact is often less visible but deeply intertwined with daily behaviours such as sleep, nutrition, energy levels, and activity levels (NICE, 2022). These factors not only influence wellbeing day to day but also shape an individual’s ability to engage in positive, meaningful change.
NHS guidance emphasises that lifestyle changes, such as improved nutrition, sleep, and hygiene, are essential to a holistic recovery plan. Yet for many individuals, the challenge is doing it consistently. For individuals experiencing anxiety and depression, even small actions like going for a walk or improving sleep can feel overwhelming.
To better understand what sustainable change looks like in this context, we analysed data from over 11,600 Holly Health users living with anxiety and/or depression, examining both baseline health behaviours and changes observed over 8 weeks and 6 months.
Baseline Health Profile
The onboarding data from this cohort (11,632 who reported a diagnosis of anxiety and/or depression) highlights the daily barriers individuals face while trying to improve their mental wellbeing. Across the cohort, low energy, poor sleep, limited physical activity, and elevated stress levels were common themes that can make simple behaviour changes feel difficult.

Multi-Condition Reality
Anxiety and depression rarely exist in isolation. Around 33.1% of users reported living with four or more health conditions, including hypertension, IBS, and chronic pain. This highlights the complexity of managing mental health issues alongside other physical health challenges.
The Hidden Burden of Stress
Stress levels were strikingly high at baseline, with 54.8% of users reporting “High” or “Very High” stress in the last two weeks. This highlights stress as a prominent feature within this population.
Energy and Sleep as Barriers to Behaviour Change
Many users reported barriers that are associated with affecting behaviour change. Around 69% indicated feeling tired most days, and 48.69% reported sleeping fewer than six hours per night. Fatigue and poor sleep are commonly associated with reduced capacity to engage in health and wellbeing-related behaviours.
Low Baseline Activity Levels
At baseline (the beginning of the Holly Health journey), 47.28% of users were below recommended levels for moderate physical activity, and over 82% were not meeting strength-based exercise guidelines. These patterns provide context when interpreting subsequent changes.
Outcomes After 8 Weeks: Measured Changes
After eight weeks of using Holly Health, we assessed changes among users with low-to-medium baseline scores who completed follow-up surveys (n=800).
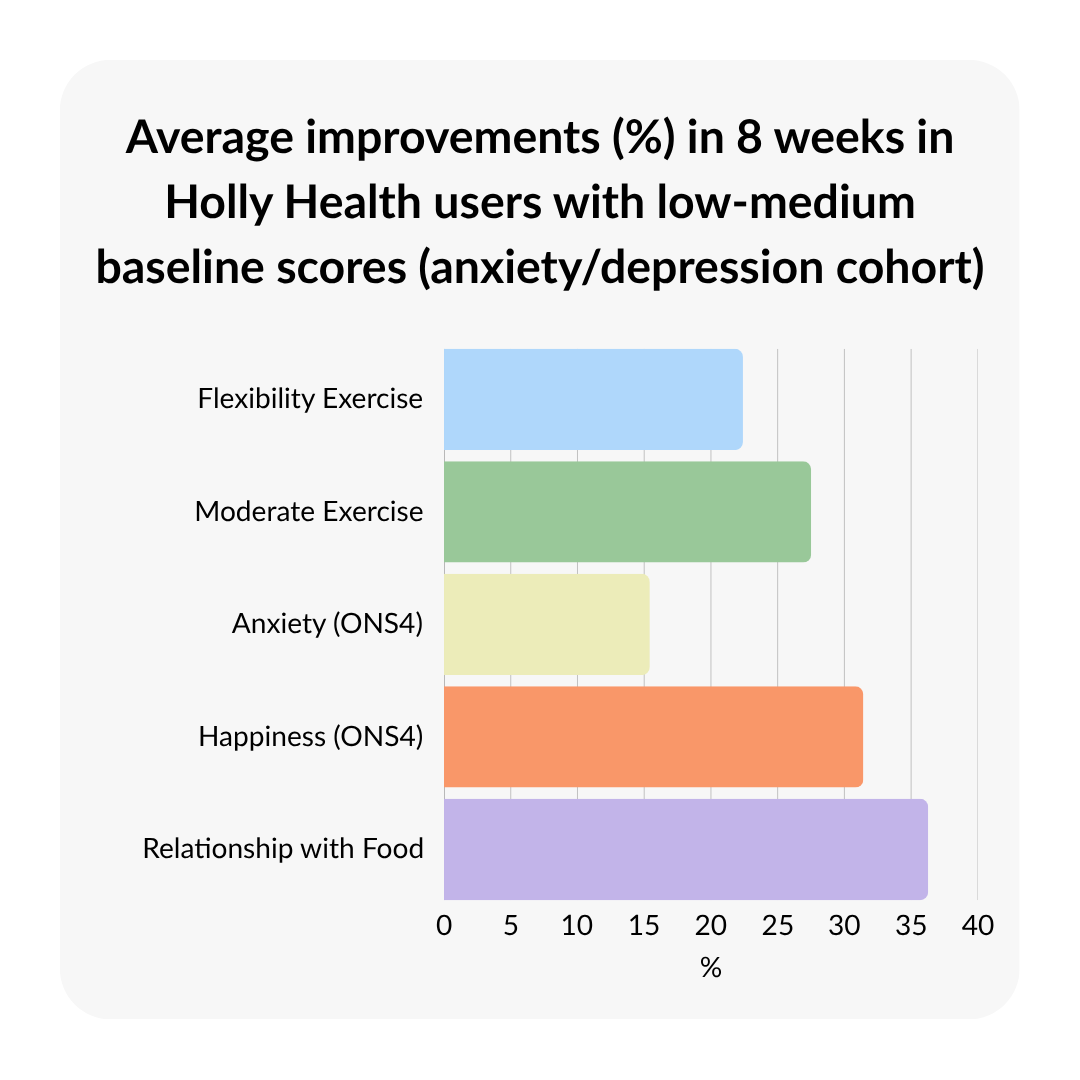
Changes in Mental Wellbeing Measures
Using the ONS personal wellbeing measures (ONS4), users showed an average improvement of 24.20% across combined wellbeing measures. Anxiety scores decreased by 15.42% (where lower scores indicate improvement), while happiness scores increased by 31.42%, and life satisfaction increased by 24.54%. These findings indicate positive shifts in self-reported wellbeing over the eight-week period.
Positive changes were also observed in physical activity. Moderate exercise increased by 27.51%, and flexibility-based activity increased by 22.40%. These improvements appear to align with the addition of simple, accessible habits such as stretching, walking, or drinking more water, rather than intensive exercise programs.
Assessing nutrition-related behaviours, users reported a 36.28% improvement in their relationship with food. This suggests an impactful shift toward more supportive eating patterns over time.
Outcomes After 6 Months: Sustained Trends
Longer-term data provide insights into whether these tangible changes were sustained or improved over time.
At six months, several trends observed at eight weeks persisted, particularly across mental wellbeing measures. Anxiety scores remained lower than baseline levels (indicating sustained reductions), while happiness increased by 31.86% and life satisfaction by 28.68%. These patterns suggest that improvements in core wellbeing measures were, for some users, sustained over a long period of time.
Additional measures also showed continued improvements. Stress levels decreased over time, while mindfulness and self-management scores increased, indicating more engagement in supportive behaviours. Physical activity levels, including both moderate and strength-based exercise, also remained higher than baseline, suggesting behavioural changes were sustained.
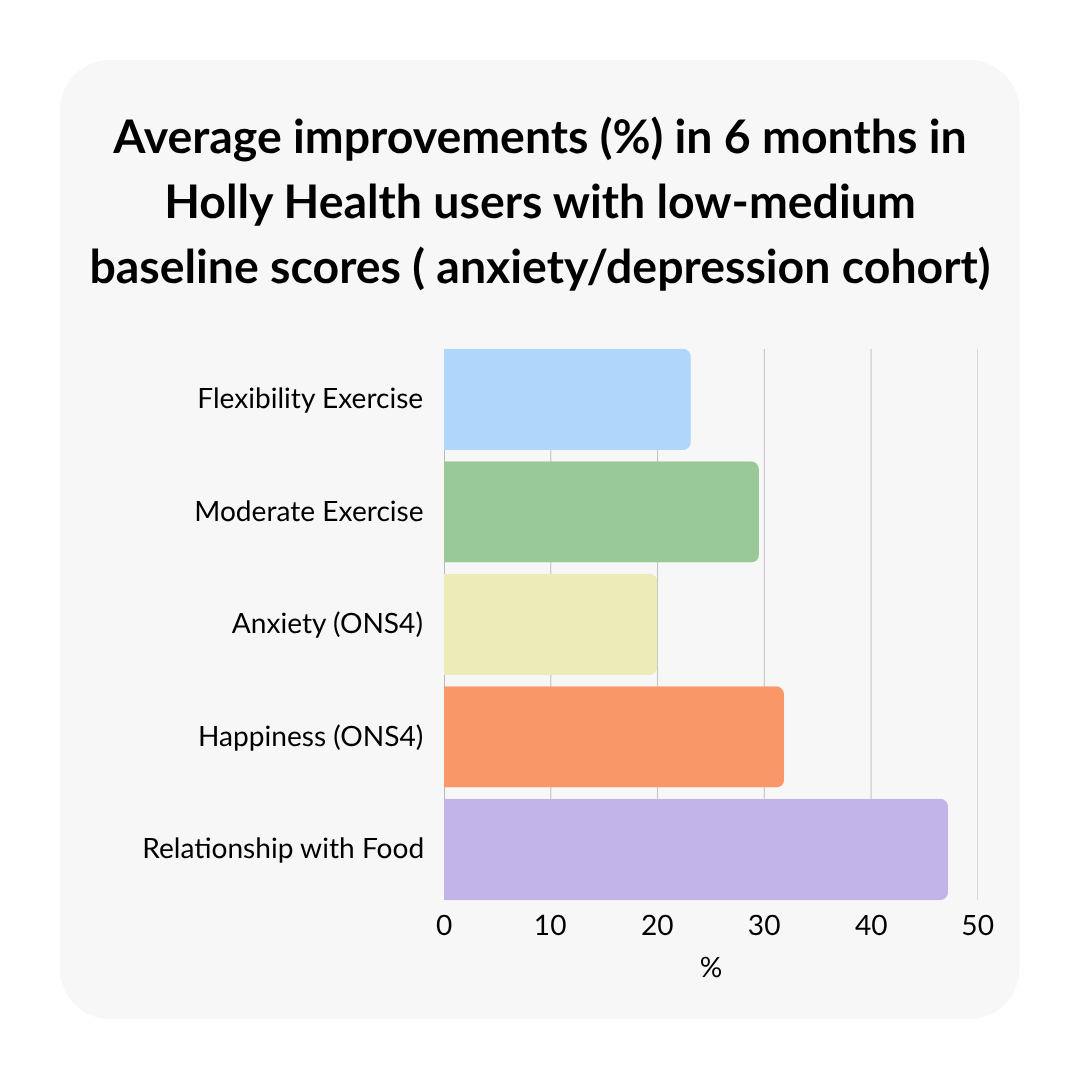
Healthcare Impact
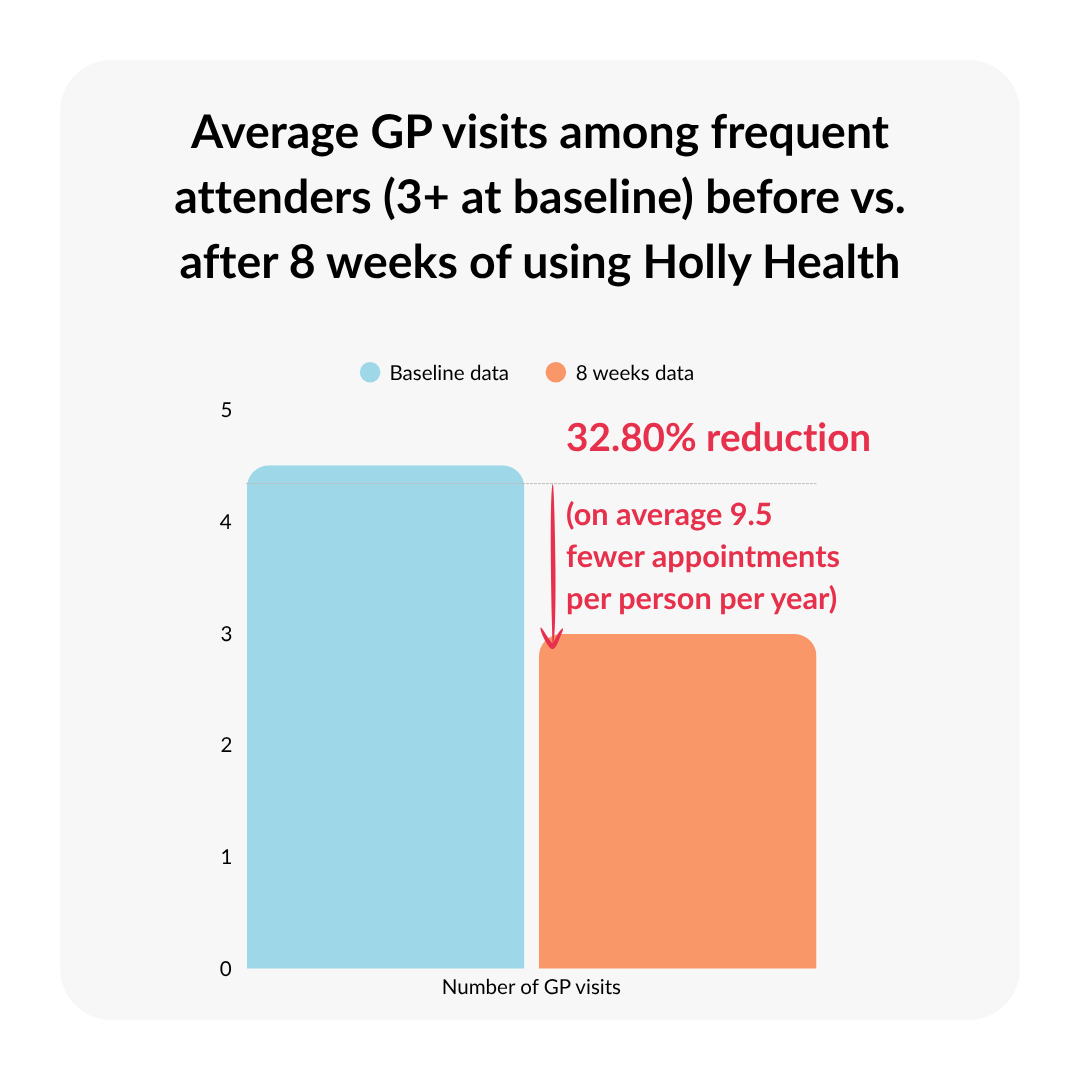
Changes were also observed in primary care usage. Among frequent attenders, who are defined as users with three or more GP appointments over an 8-week period at baseline, GP visits decreased by 32.80% at 8 weeks with reductions reaching 40.04% at 6 months. This corresponds to an average reduction of 1.46 appointments over 8 weeks, which translate to a potential reduction of approximately 9.5 appointments per person per year. These findings point toward increased self-management for the user as well as the potential for significant cumulative savings in clinical time and a reduced burden on primary care infrastructure.
Real Voices: User Reflections
User feedback provides additional context to the quantitative findings, highlighting how small changes can translate to everyday shifts.
Several users described becoming more active and building manageable routines in their daily lives. One user shared that Holly Health supported them in making “small, achievable, lasting changes” that helped them move more and reduce feelings of fatigue.

Others reflected on shifts in perspective, describing a greater focus on “what they can do rather than what they can’t do.

Users also highlighted improvements in self-reflection. For example, one noted an increased ability to reflect positively on themselves through practices like journaling. This indicates the role of small habits in supporting mental wellbeing.

Conclusion
This analysis of 11,632 Holly Health users with depression and/or anxiety provides insight into how small behaviour changes are associated with physical and mental changes over time.
The observed 24.20% improvement in combined wellbeing scores at 8 weeks, alongside sustained trends at 6 months, suggests that structured support for adopting new health habits can play a role in supporting individuals with anxiety and depression.
By focusing on manageable adjustments, from drinking more water to practising mindfulness, users have shown to make impactful shifts in reclaiming their energy and building a foundation for long-term recovery and sustainability, best put from a Holly Health user: "Start out with small steps... Give it a go. You will have good days and bad. This is normal. Don't give up, you have got this."












